What is impaired hemostasis
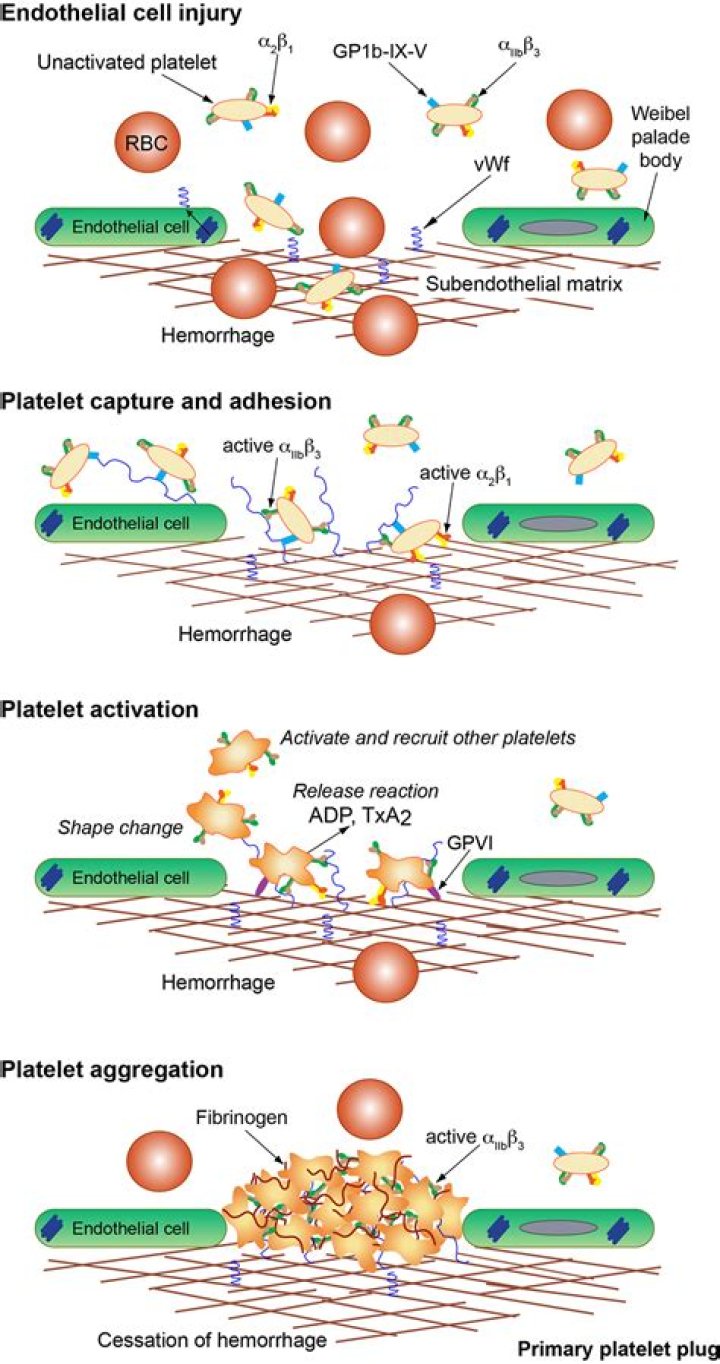
Clinical signs of primary hemostatic disorders include petechiae, mucosal hemorrhage, prolonged bleeding at sites of injury.
What are symptoms of hemostasis?
Clinical signs of primary hemostatic disorders include petechiae, mucosal hemorrhage, prolonged bleeding at sites of injury.
What is a hemostasis disorder?
Hemostatic disorders occur in all pathways of hemostasis and can be inherited or acquired. They are usually recognized clinically by excessive hemorrhage. History, signalment and clinical signs can guide a clinician as to the likely underlying disorder.
What is inadequate hemostasis?
Achieving perioperative hemostasis is vital to surgical success. Inadequate control of bleeding is associated with serious adverse outcomes, including extended duration of surgery, unanticipated blood transfusions, shock, infection, impaired wound healing, longer hospital stays, and mortality.What causes abnormal hemostasis?
Numerous hemostatic abnormalities have been associated with acute and chronic renal disease. The most common abnormalities are defective platelet aggregation, decreased platelet adhesiveness, decreased platelet factor-3 availability, and prolongation of the bleeding time.
Is hemostasis a blood clot?
Hemostasis refers to normal blood clotting in response to an injury. However, your body can also have too much clotting, known as hypercoagulability. That can cause many blood clots to form spontaneously and block normal blood flow.
What stage of hemostasis is affected by aspirin?
The primary established effect of aspirin on hemostasis is to impair platelet aggregation via inhibition of platelet thromboxane A2 synthesis, thus reducing thrombus formation on the surface of the damaged arterial wall.
What is the function of hemostasis?
Hemostasis is the mechanism that leads to cessation of bleeding from a blood vessel. It is a process that involves multiple interlinked steps. This cascade culminates into the formation of a “plug” that closes up the damaged site of the blood vessel controlling the bleeding.How does hemophilia affect hemostasis?
Hemophilia is caused by a mutation or change, in one of the genes, that provides instructions for making the clotting factor proteins needed to form a blood clot. This change or mutation can prevent the clotting protein from working properly or to be missing altogether.
What is tertiary hemostasis?Tertiary hemostasis is defined as the formation of plasmin, which is the main enzyme responsible for fibrinolysis (breakdown of the clot). At the same time as the coagulation cascade is activated, tissue plasminogen activator (tPA) is released from endothelial cells.
Article first time published onHow can vitamin K deficiency affect hemostasis?
Both calcium and vitamin K are needed to synthesize Protein C, an anticoagulant that prevents excessive coagulation after the coagulation cascade occurs. Deficiency of any of these clotting cofactors will cause an impaired ability for blood to coagulate, which can contribute to excessive bleeding and hemorrhage.
What is coagulation dysfunction?
Coagulation disorders are disruptions in the body’s ability to control blood clotting. Coagulation disorders can result in either a hemorrhage (too little clotting that causes an increased risk of bleeding) or thrombosis (too much clotting that causes blood clots to obstruct blood flow).
What causes blood to thin out?
Thin blood is known as thrombocytopenia and is caused by low numbers of platelets. The normal level of platelets in the blood is between 150,000–400,000 per milliliter (mL) . If levels of platelets fall below 150,000/mL, it may indicate thin blood.
How are blood clotting disorders treated?
Medications are the main treatment for clotting disorders. They include: Anticoagulants, commonly called blood thinners, may be given intravenously (IV) or in your child’s vein. Aspirin may be used with anticoagulants.
What is the difference between bleeding disorder and clotting disorder?
For blood to clot, your body needs cells called platelets and proteins known as clotting factors. If you have a bleeding disorder, you either do not have enough platelets or clotting factors or they don’t work the way they should.
Is a leg blood clot serious?
This condition can lead to several health issues, including pain, swelling, cramps, varicose veins, leg ulcers, and blood clots in the legs. Blood clots in the legs are especially serious since they can trigger a potentially fatal medical emergency called a pulmonary embolism.
What are the signs and symptoms of platelet function disorders?
- Easy bruising.
- Nosebleeds.
- Heavy periods.
- Bleeding gums when baby teeth fall out.
- Bleeding into the gut.
- Excessive bleeding during surgery or after minor injuries.
Does aspirin affect homeostasis?
Aspirin’s effect on homeostasis is well-known. Low-dose aspirin (acetylsalicylic acid, 81 mg) inhibits the enzyme Cox-1, which produces thromboxane A-2, necessary for platelet aggregation.
How does aspirin prevent the formation of thrombi?
Aspirin prevents thrombi formation by blocking platelet production of thromboxane A2, an essential platelet aggregation component. Aspirin has the ability to suppress the creation of prostaglandins and thromboxane A2 by irreversibly inactivating the cyclooxygenase-1 (COX-1) enzyme.
How do you get hemostasis?
A variety of hemostatic methods can be employed, ranging from simple manual pressure application with one finger to electrical tissue cauterization, systemic administration of blood products, and systemic administration or topical application of procoagulation agents.
What are the stages of homeostasis?
There are three stages of homeostasis. They are sensing, processing and responding. These stages are managed by the receptor, control center and effector respectively.
Which cell is responsible for your hemostasis?
Normal hemostasis is the responsibility of a complex system of three individual components: blood cells (platelets), cells that line the blood vessels (endothelial cells), and blood proteins (blood-clotting proteins). The blood platelet is a nonnucleated cell that circulates in the blood in an inactive, resting form.
How does hemophilia affect the cardiovascular system?
Hemophilia and CVD. Because both elevated levels of clotting factor VIII and VWF increase the risk of arterial thrombosis,2,3 hemophilia, which is associated with a lifelong hypocoagulable state, may theoretically offer protection against CVD (ie, acute coronary syndrome, stroke, or peripheral vascular disease).
What mutation causes hemophilia?
Changes in the F8 gene are responsible for hemophilia A, while mutations in the F9 gene cause hemophilia B. The F8 gene provides instructions for making a protein called coagulation factor VIII. A related protein, coagulation factor IX, is produced from the F9 gene.
What type of mutation is hemophilia?
Hemophilia is inherited in an X-linked recessive pattern. A condition is considered X-linked when gene mutation that causes it is located on the X chromosome, one of the two sex chromosomes. In males (who have only one X chromosome), one altered copy of the gene in each cell is enough to cause the condition.
What is homeostasis and Haemostasis?
Hemostasis and homeostasis are two processes that maintain the proper functioning of the body. Hemostasis prevents the blood loss from the circulation system while homeostasis maintains a constant internal environment.
How does hemostasis affect platelets?
Released secretary granules will recruit additional platelets to form the platelet plug, which is referred to as primary hemostasis10. Following vasoconstriction, exposed collagen from the damaged surface will encourage platelets to adhere, activate and aggregate to form a platelet plug, sealing off the injured area.
What is the difference between hemostasis and coagulation?
Coagulation (or clotting) is the process through which blood changes from a liquid and becomes thicker, like a gel. Coagulation is part of a larger process called hemostasis, which is the way that the body makes bleeding stop when it needs to.
What are fibrin strands?
Fibrin is a tough protein substance that is arranged in long fibrous chains; it is formed from fibrinogen, a soluble protein that is produced by the liver and found in blood plasma. When tissue damage results in bleeding, fibrinogen is converted at the wound into fibrin by the action of thrombin, a clotting enzyme.
What is hemostasis in cattle?
Hemostasis is a complex physiological process involving cells (platelets, especially but also fibroblasts), and soluble (coagulation factors and inhibitors) and insoluble proteins (extracellular matrix proteins).
What is secondary hemostasis?
Secondary hemostasis refers to the cascade of enzymatic reactions that ultimately results in the conversion of fibrinogen to fibrin monomers. Fibrin monomers are then cross-linked into insoluble strands that serve to stabilize the loose platelet clot formed in primary hemostasis.