What is prone body position
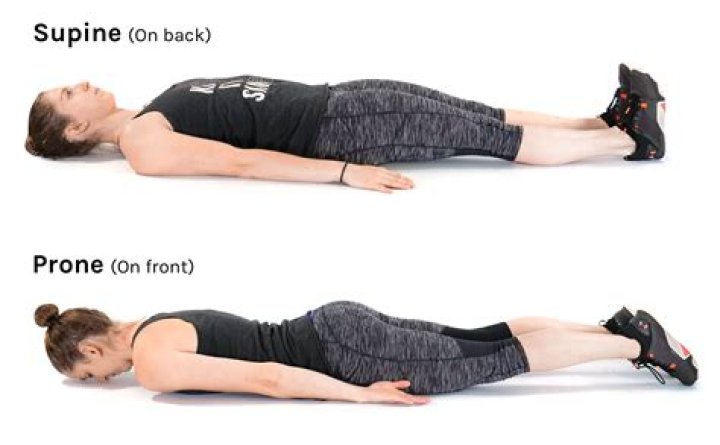
According to Nancy, proning is the process of turning a patient with precise, safe motions from their back onto their abdomen (stomach) so the individual is lying face down.
What is prone position for patients suffering from COVID-19?
Hospitalized patients typically lie on their backs, a position known as supine. In prone positioning, patients lie on their abdomen in a monitored setting. Prone positioning is generally used for patients who require a ventilator (breathing machine).
How does a ventilator help with breathing problems of COVID-19?
When your lungs inhale and exhale air normally, they take in oxygen your cells need to survive and expel carbon dioxide. COVID-19 can inflame your airways and essentially drown your lungs in fluids. A ventilator mechanically helps pump oxygen into your body.
How long does someone typically stay on a ventilator due to COVID-19?
Some people may need to be on a ventilator for a few hours, while others may require one, two, or three weeks. If a person needs to be on a ventilator for a longer period of time, a tracheostomy may be required. During this procedure, a surgeon makes a hole in the front of the neck and inserts a tube into the trachea.When can COVID-19 symptoms begin to appear?
Symptoms may appear 2-14 days after someone is exposed to the virus and can include fever, chills, and cough.
What are the most used breathing aid devices for COVID-19?
Breathing aid devices are used to support the patients who have acute respiration problem due to pneumonia associated diseases like COVID-19, asthma, and dry coughing. The most used devices which are utilized for COVID-19 treatment are oxygen therapy device, ventilator, and CPAP device.
How long can a patient still feel the effects of COVID-19 after recovery?
Older people and people with many serious medical conditions are the most likely to experience lingering COVID-19 symptoms, but even young, otherwise healthy people can feel unwell for weeks to months after infection.
What are symptoms of COVID-19 affecting the lungs?
Some people may feel short of breath. People with chronic heart, lung, and blood diseases may be at risk of severe COVID-19 symptoms, including pneumonia, acute respiratory distress, and acute respiratory failure.In what circumstances are ventilators needed for patients with COVID-19?
For the most serious COVID-19 cases in which patients are not getting enough oxygen, doctors may use ventilators to help a person breathe. Patients are sedated, and a tube inserted into their trachea is then connected to a machine that pumps oxygen into their lungs.
What is the recovery time for COVID-19 patients with Acute Respiratory Distress Syndrome (ARDS)?Most people who survive ARDS go on to recover their normal or close to normal lung function within six months to a year. Others may not do as well, particularly if their illness was caused by severe lung damage or their treatment entailed long-term use of a ventilator.
Article first time published onWhat happens to your lungs if you get a critical case of COVID-19?
In critical COVID-19 — about 5% of total cases — the infection can damage the walls and linings of the air sacs in your lungs. As your body tries to fight it, your lungs become more inflamed and fill with fluid. This can make it harder for them to swap oxygen and carbon dioxide.
Do all patients with COVID-19 get pneumonia?
Most people who get COVID-19 have mild or moderate symptoms like coughing, a fever, and shortness of breath. But some who catch the new coronavirus get severe pneumonia in both lungs. COVID-19 pneumonia is a serious illness that can be deadly.
How long is the incubation period for COVID-19?
– The incubation period for COVID-19. Given that the incubation period can be up to 14 days, CDC recommends conducting screening testing at least weekly.
What are some of the common symptoms of the COVID-19 disease?
Symptoms may include: fever or chills; cough; shortness of breath; fatigue; muscle and body aches; headache; new loss of taste or smell; sore throat; congestion or runny nose; nausea or vomiting; diarrhea.
What happens if a recovered person from COVID-19 develop symptoms again?
If a previously infected person has recovered clinically but later develops symptoms suggestive of COVID-19 infection, they should be both quarantined and retested.
Can you experience recurring COVID-19 symptoms during the recovery process?
Yes. During the recovery process, people with COVID-19 might experience recurring symptoms alternating with periods of feeling better. Varying degrees of fever, fatigue and breathing problems can occur, on and off, for days or even weeks.
Could deep breaths and forced coughs help treat COVID-19?
DEEP breaths and forced coughs could help clear mucus but are unlikely to help people with a dry cough and mild cases of covid-19, despite what advice on social media would have you believe. Breathing exercises help manage some respiratory conditions, like chronic obstructive pulmonary disease.
What is Continuous Positive Airway Pressure (CPAP) for COVID-19?
Continuous Positive Airway Pressure is a well-known device that is used for breathing assistant for the treatment of patients having a mild respiratory problem. The positive airway pressure is delivered through a tight face or nasal mask in CPAP device.
Which medications can help reduce the symptoms of COVID-19?
In terms of specifics: acetaminophen (Tylenol), naproxen (Aleve) or ibuprofen (Advil, Motrin) can help lower your fever, assuming you don’t have a health history that should prevent you from using them. It’s usually not necessary to lower a fever – an elevated temperature is meant to help your body fight off the virus.
Is shortness of breath an early symptom of Pneumonia due to COVID-19?
Breathlessness is caused by an infection in the lungs known as pneumonia. Not everyone with COVID-19 gets pneumonia, though. If you don’t have pneumonia, you probably won’t feel short of breath.
What SpO2 oxygen level is normal for COVID-19 patients?
An SpO2 of 100% has effectively zero clinical difference to a 96% reading. As a good rule of thumb, a person with COVID-19 monitoring his or her clinical status at home will want to ensure that the SpO2 reading stays consistently at or above 90 to 92%.
How long does it take for the body to produce antibodies against COVID-19?
Antibodies can take days or weeks to develop in the body following exposure to a SARS-CoV-2 (COVID-19) infection and it is unknown how long they stay in the blood.
Can the coronavirus disease cause breathing problems?
COVID-19 is a respiratory disease, one that especially reaches into your respiratory tract, which includes your lungs. COVID-19 can cause a range of breathing problems, from mild to critical.
Is COVID-19 lung damage reversible?
After a serious case of COVID-19, a patient’s lungs can recover, but not overnight. “Recovery from lung damage takes time,” Galiatsatos says. “There’s the initial injury to the lungs, followed by scarring.
Is tightness in your chest a symptom of COVID-19?
Severe allergies can make you can feel tightness in your chest and shortness of breath, especially if you have asthma, too. But these can also be serious symptoms of COVID-19. If you aren’t sure or if you haven’t been diagnosed with asthma, call your doctor or 911 right away.
How long does it take to recover from COVID-19?
Fortunately, people who have mild to moderate symptoms typically recover in a few days or weeks.
Can COVID-19 cause acute respiratory distress syndrome?
Lung damage in the course of this disease often leads to acute hypoxic respiratory failure and may eventually lead to acute respiratory distress syndrome (ARDS). Respiratory failure as a result of COVID-19 can develop very quickly and a small percent of those infected will die because of it.
Is COVID-19 linked to acute respiratory distress syndrome (ARDS) and multi-organ dysfunction?
The significant mortality rate associated with the ongoing Coronavirus disease 2019 (COVID-19) pandemic has been linked to acute respiratory distress syndrome (ARDS) and multi-organ dysfunction. Mechanisms underlying the phenomenon remain unclear.
What happens to the body during a COVID-19 critical infection?
During a severe or critical bout with COVID-19, the body has many reactions: Lung tissue swells with fluid, making lungs less elastic. The immune system goes into overdrive, sometimes at the expense of other organs. As your body fights one infection, it is more susceptible to additional infections.
Can COVID-19 damage organs?
UCLA researchers are the first to create a version of COVID-19 in mice that shows how the disease damages organs other than the lungs. Using their model, the scientists discovered that the SARS-CoV-2 virus can shut down energy production in cells of the heart, kidneys, spleen and other organs.